Anatomy
The stomach of the horse is small compared to other species, its capacity is only 10-15 litres. The stomach sits in the abdomen beneath the rib cage, food comes from the mouth down the oesophagus (food pipe) and enters the stomach through the cardiac opening. In humans the stomach and the oesophagus have two different linings, the stomachs lining is known as the glandular lining and the oesophageal lining as the squamous cell lining. In horses the oesophageal squamous cell lining extends into the upper half of the stomach and the margin where this meets the glandular mucosa is called the margo plicatus. Food leaves the stomach via the Pylorus (a muscular sphincter) and enters the duodenum (small intestine).
Physiology
The glandular part of the stomach produces hydrochloric acid at a rate of 1.5L/hour which is a very strong acid (200x acidity of vinegar) and kills some bacteria and other germs that have been ingested (eaten) with food and might otherwise be harmful. The acid release is stimulated by the hormones histamine and gastrin. A horse’s stomach continuously produces acid because they are designed to eat for most of the day. The stomach also produces enzymes to digest food which results in a release of organic acids from the broken down food that contributes to the acidic environment. This acid would also damage the delicate stomach lining if it wasn’t for some clever protective mechanisms which include;
- Saliva; saliva contains a lot of bicarbonate which is alkaline (high pH) and neutralises the acid. Its main protective effect is in the squamous region at the top of the stomach as the saliva enters the stomach here with the food.
- Bicarbonate and mucus secretion; released from the lining of the glandular stomach, the mucus dilutes the acid and the bicarbonate neutralises it, together forming a protective lining. The pH measured immediately adjacent to the stomach lining is neutral where as in the middle of the gastric contents it will be pH2-3. Bicarbonate and mucous secretion are stimulated by hormones called prostaglandins.
- The cells lining the squamous region are tightly held together by strong bonds so there is no chance of stomach contents leaking between the cells.
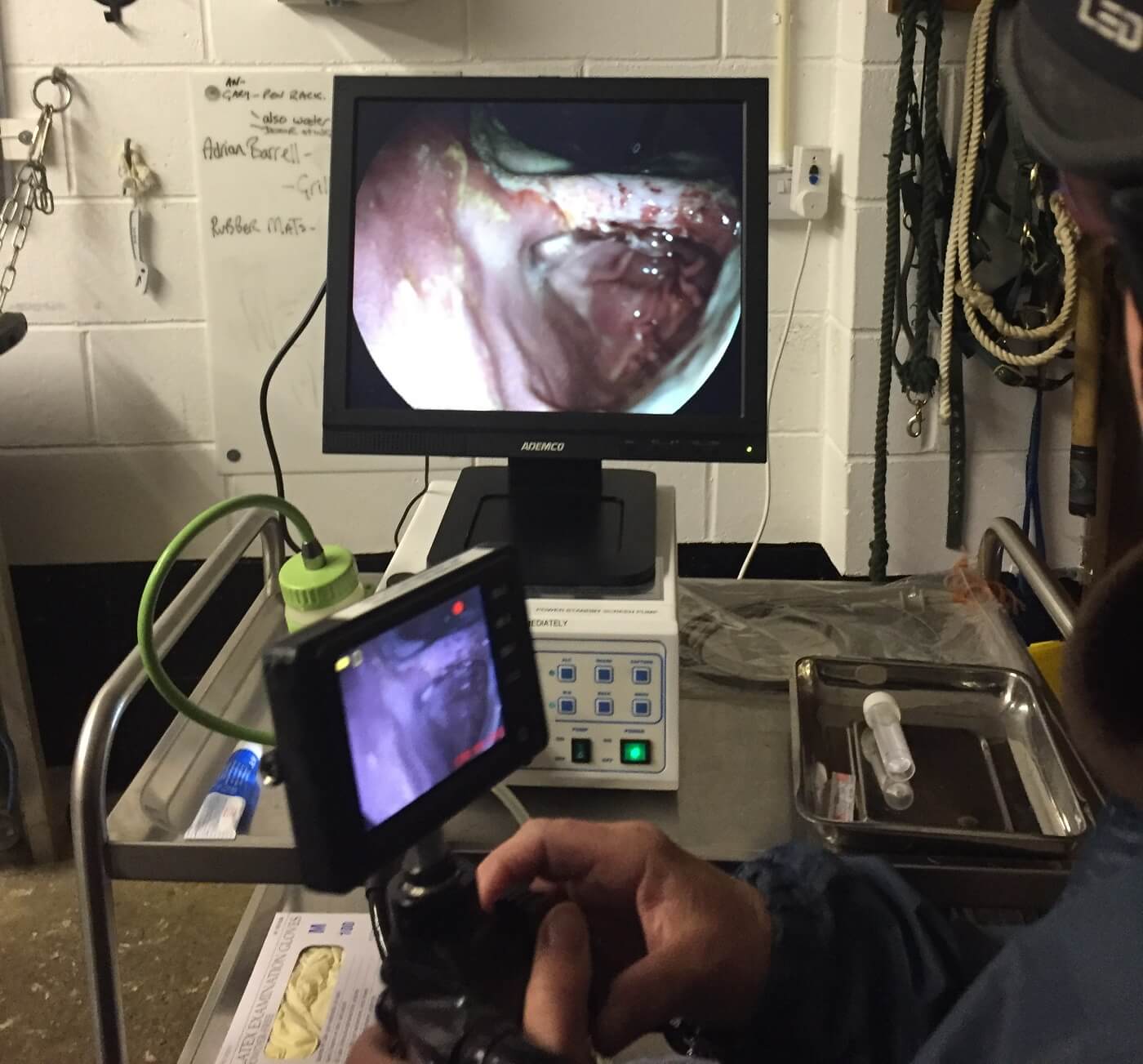
Grade 4 Squamous ulcers on the screen using Deben Valley’s Gastroscope
Cause of Gastric Ulcers
Ulcers in the squamous region form due to prolonged exposure to acid. This can come about for several reasons. More acid is produced when high volumes of carbohydrates are fed because these are partially digested in the stomach to release organic fatty acids. Carbohydrate rich cereals require less chewing than fibrous hay; the less time spent chewing means the less saliva is produced to buffer the stomach acid. This is one of the key reasons that horses in training get gastric ulcers.
Exercising at high speeds causes physical disruption of the stomach contents which normally lies in a carefully stratified way with a fibrous mat at the top that prevent the acid contents below reaching the squamous region. At high speeds, the stomach contents become more mixed and acid splashes against the squamous region causing ulcers.
True ulcers rarely form in the glandular region; the disease we see here is much more of a gastritis (inflammation) and is known as gastric glandular disease. This disease is caused when there is a disturbance in the balance between acid production and mucosal protective mechanisms. The prostaglandins that stimulate production of mucus and bicarbonate in the glandular region can be inhibited by;
- Cortisol; released by the body in response to stress
- Drugs in the group known as NSAIDS e.g. Bute, Flunixin
When exercising the blood flow to the stomach decreases which also reduces the amount of mucus and bicarbonate that can be produced. A reduction in mucus and bicarbonate production reduces the buffering capacity of the stomach wall and exposes the glandular region to acid.
Risk Factors
- Carbohydrate rich diet
- Long periods of fasting
- Restricted turn out
- Periods of withdrawal from water
- Stressful environment (psychological stress)
- Stressful activities like travelling, and for some horses box rest
- Fast exercise
- Some drugs
- Problems of gastric motility
- Wind sucking or crib biting
- Other diseases and pain

Incidence of Gastric Ulcers
The following percentages are the proportion of horses engaged in different activities that will have gastric ulcers.
- 37% Leisure horses
- 63% Performance horses
- 93% Race horses
- 50% Foals, even horses turned away in fields can suffer gastric ulcers
Symptoms
- Weight loss
- Bloated abdomen
- Dull coat
- Picky and slow eating
- Recurrent colic / lays down after or during eating
- Poor performance
- Depression and attitude changes ‘GRUMPY’
- Behavioural changes
- Wind sucking or crib biting
- Teeth grinding
- “Girthy” – pulls faces and moves away when the girth is done up
- Bracing of the back when saddled/ridden (‘cold-backed’). This can progress from reluctance to go forward to bucking/rearing.
- Adopting unusual stances such as stretching or laying down in odd positions
- Spookiness / random unexpected behaviour under saddle for no obvious reason
- Diarrhoea
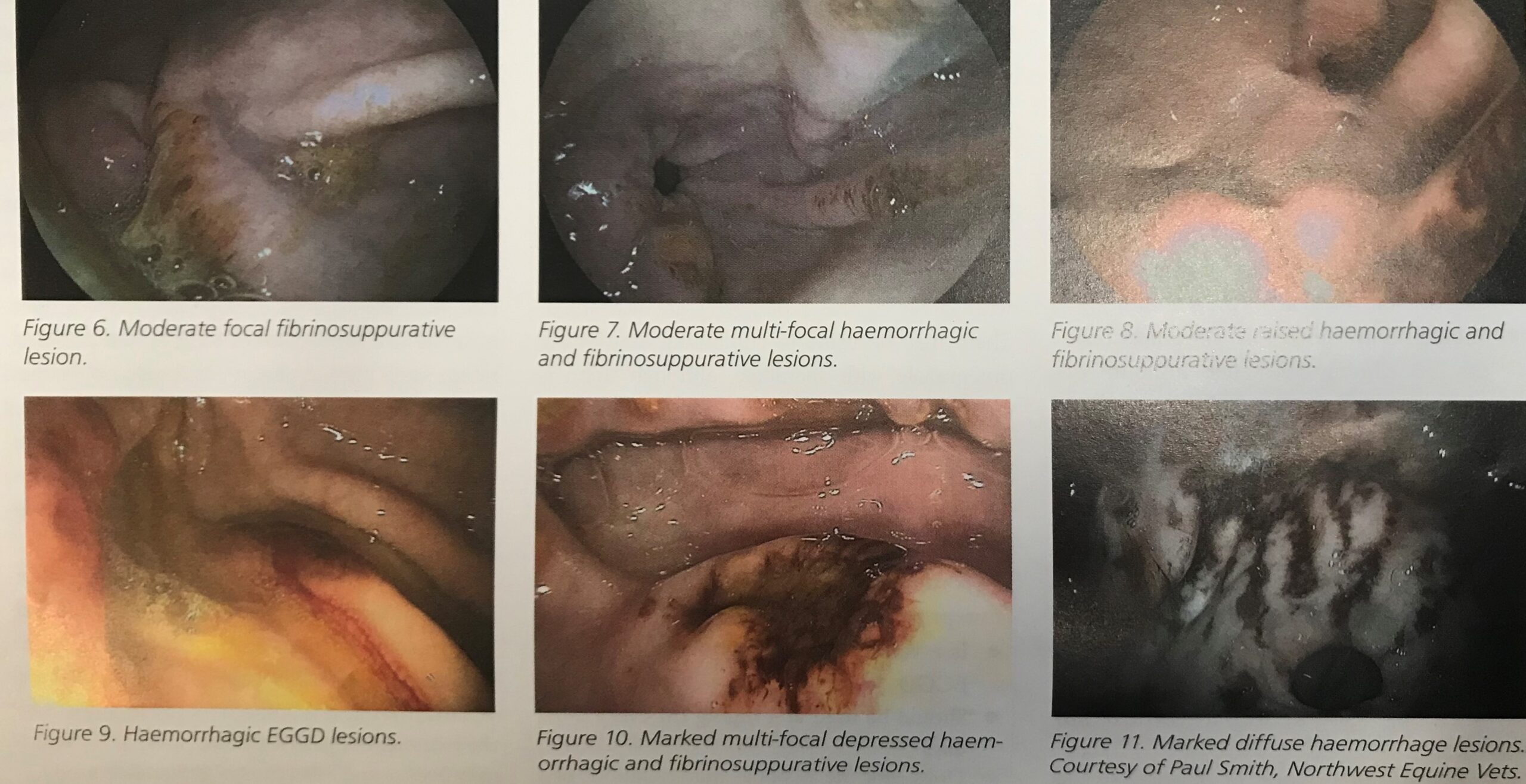
Examples of Equine Gastric Glandular Disease
Quotes from Owners of Horses with Gastric Ulcers
I am six weeks on from my mare’s scope which found nasty grade 2 and grade 3 ulcers. Her only symptoms were girthyness, inability to maintain weight and general tension/spookyness/unexploded bomb like attitude. Testing and treating Holly has caused the most amazing transformation in her whole outlook, although she is still a bit of a wazzock at times she is softer, more friendly, calmer, more rational and a whole heap fatter! (in a good way – was all ribs and bones by the time I scoped her).
I was told all the time that Nancy was fat because she had the HUGE belly, she really swelled out behind the girth area, she actually looked in foal, she had no fat on her bum, her back or her neck (although she was by no means skinny), and I could feel her ribs so I knew she wasn’t ‘officially overweight. anyway, it turns out she had ulcers and a few days after starting treatment the ‘bloatedness’ went and she started to look like she had abs again, and now the ulcers have gone she looks great.
He has always been a very picky eater and takes ages to finish. After eating his feed he often lies down and stretches, sometimes he even groans. Sometimes when being ridden he just suddenly stops and looks like he wants to wee but he never does. When he was scoped we found grade 3 ulcers and after treatment, all his symptoms went away and he had never looked so good
He paws at his bed during the night, doesn’t always finish his hard feed in one go, doesn’t actually eat that much haylage, if you put more in then he drags into bed (kind of like he wants to eat it but is frustrated that he can’t) he quite often spends time standing in the field without eating, he has to bite something when I do the girth up – even if I do it extremely loosely and I think this has got slightly worse recently.
I have just had my welsh cob scoped, always looked well, never off his food, shiny coat etc. He lives out 24/7 in a herd, has a stress free life and has been like that for 6 years. The thing that made me scope him is he reacts to having a saddle put on and is uptight when ridden. He was given to us as he had bolted and had a saddle under his belly so he has reasons to be worried!
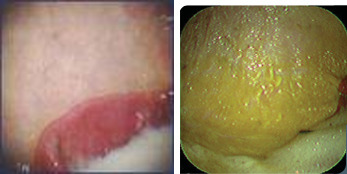
Normal squamous surface Grade 1 ulceration (yellow and thickened stomach lining
Diagnostics
The gold standard technique for diagnostics is Endoscopy with a 3 metre gastroscope.
Endoscopy involves putting a small video camera on the end of a long cable into the stomach via the nose and food pipe to look for ulcers in the stomach lining. The most common places ulcers are found are around the margo plicatus (junction of the glandular and squamous lining) and near the pylorus. The procedure its-self straight forward and takes about 30mins to perform. In order to get a good view of the stomach lining whilst Endoscopy is performed the stomach needs to be empty of food. To ensure the stomach is empty enough the horse needs to be starved for 18-20 hours and have water removed at least 4 hours prior to the procedure.
Horses will be sedated for gastroscopy so time will need to be allowed for them to wake up (approximately 1 hour) after the procedure before they travel home. Ideally they will eat a feed and some forage; have plenty of gut sounds are passed dung before they leave the clinic.
Risks involved with the procedure include nose bleeds from passing the scope up the nose, these will stop on their own within 5 minutes, and colic from the combination of fasting and sedation. Horses are monitored carefully for colic before and after the procedure so if it occurs it can be treated quickly.
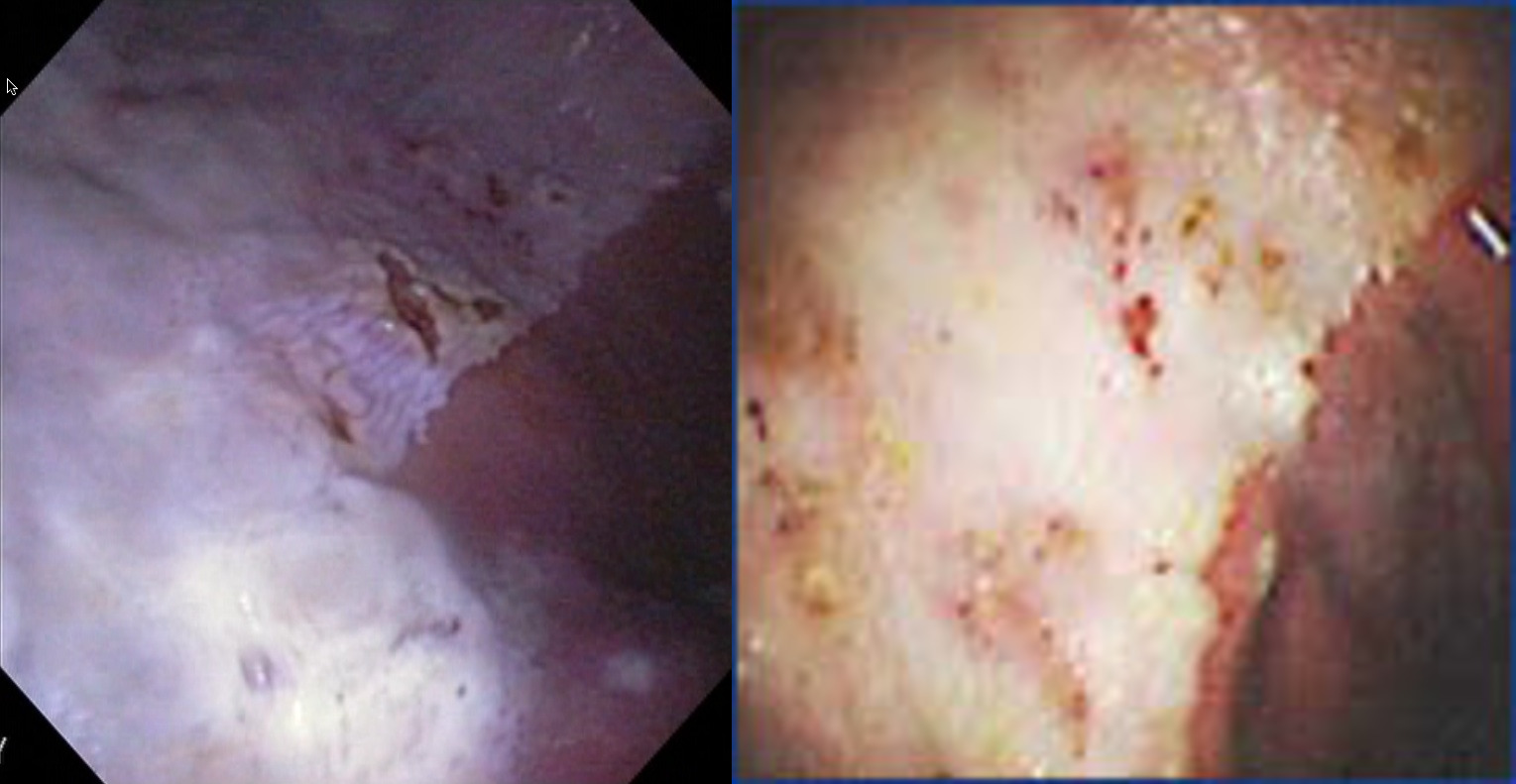
Grade 2 ulceration Grade 3 ulceration – squamous
Grading
When squamous ulcers are diagnosed they are graded on a scale of 0-4 depending on their severity
Grade 0 Normal
Grade 1 Mild reddening or thickening
Grade 2 Small single or small multifocal lesions
Grade 3 Large single or multifocal lesions or extensive multifocal lesions
Grade 4 Extensive (often coalescing) lesions with areas of deep ulceration
It should be noted that severity of ulcers does not correlate well with severity of clinical signs.
Glandular disease is categorised by the appearance of the inflammation and the lesions are described as:
- Focal, multi-focal or diffuse
- Mild, moderate or severe
- Nodular, raised, flat or depressed
- erythematous, haemorrhagic or fibrinosupparative
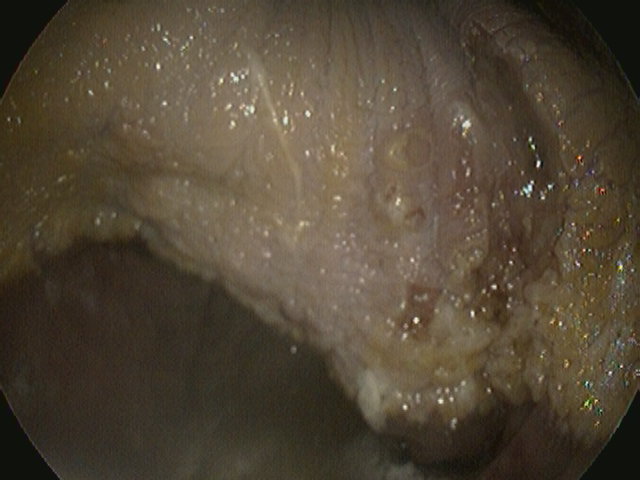
Squamous ulceration grade 4 – bleeding
Treatment
Treatment requires a multi targeted approach. Of course, the first place to start is to try and remove the cause of the ulcers in the first place. This often means making considerable management changes like increasing the amount of turn out time, changing the diet and possibly changing yards. It is tempting to think that by turning a horse with gastric ulcers out to pasture all the time the ulcers will heal with no other assistance. Unfortunately, this is not the case. Horses with ulcers have been turned out, given only fibre feeds and not ridden and this still does not heal the ulcers – this is really relevant to the most common type of ulcers caused by stress and prolonged fasting. If ulcers have been caused by drugs then they do usually improve once the drug is stopped.
Therefore, in the short term medicines are used to heal the ulcers but long term, management changes to make the horse’s life style, as low risk as possible are key.
We recommend the fairfax girth for horses who have suffered gastric ulcers / disease.
For horses with glandular disease, a minimum of 2 rest days per week is recommended.
Feeding
- Increase the time spent eating/frequency of feeding – dilute the energy density of the meal
- Decrease carbohydrate intake – feed less than 1g/kg starch/meal and less than 2g/kg starch per day. Feed concentrates as several small feeds throughout the day and include fibre (alfalfa good as high in calcium).
- Increase roughage and oil intake, feed mixed forages (grass/hay/haylage) that contain low energy (protein). Forage eating time can be increased by putting the feed in haylage nets or even two hay nets (80% of feed between 7am and 7pm ideally).
- Avoid feeding straw as forage and eliminate it as a bedding material if the horse eats from its bed.
- 100-200 ml of corn oil/day, start at 5ml twice daily and slowly increase.
- Provide as much pasture turn out as possible and always provide water when at pasture.
- When supplementing pasture with hay spread the hay out as much as possible.
- If a horse has to be transported provide forage on the journey and immediately upon arrival at the destination.
- Feed fibre before exercise e.g. a double handful, about 2 litres of alfalfa 20 minutes prior to exercise which will form a protective layer at the top of the stomach and help stop splashing. Don’t over wet feed, dry feed stimulates more saliva production.
- Speak to a nutrition helpline, e.g. Saracens or Baileys.
Last reviewed March 2021.
Medication
Omeprazole is the only one drug licensed for the treatment of EGUS. It is sold under several trade names Gastrogard / Peptizole and the drug is supplied as a paste in syringes that are given to the horse by mouth – just like wormers. There is very good evidence to show that this drug works. It allows the ulcers to heal by directly inhibiting release of acid into the stomach. A standard dosing protocol would be to treat on full dose for 4 weeks and then repeat the gastroscopy. It is expected that an improvement will be seen and the dose of omeprazole is then reduced but continued for at least another fortnight. Severe ulcers and gastric glandular disease are likely to require a longer treatment time or a different drug regime. Omeprazole can be given for prevention of EGUS and is often used prior to travelling susceptible individuals. If ulcers persist beyond their expected healing time then occasionally antibiotics may be given as bacterial involvement may be suspected in refractory cases. Glandular disease require a more complicated treatment approach. Injectable Omeprazole / Prostaglandins / Sucralfate may be used under the cascade system and your vet’s guidance for glandular gastric disease.
Ranitidine is a drug that inhibits histamine release. As histamine causes a release of gastric acid ranitidine can be used to reduce acid secretion but as there are other mechanisms of acid release it is not as good as omeprazole. Ranitidine has proven to be useful in preventing ulcers during times of stress and when other drugs are given, especially in foals on anti-inflammatories. Recently it’s use has diminished.
The supplement Pro-nutrin is a combination of pectin, glycerine and lecithin and comes in a formula of small pellets that are added to feed. Pro-nutrin reduces gastric acidity by neutralisation and stabilises the protective mucous layer. Improvement and healing of ulcers following its use without other therapies have been documented using follow up endoscopic exam. Sugarbeet contains pectin.
Antacids can be given to increase the pH in the stomach but they have to be given frequently as food is continuously passing through and taking them away with it. Aluminium hydroxide comes in a commercial preparation known as Sucrulfate. This binds to the surface of the ulcer a bit like a plaster. Clinical improvement of symptoms may be seen when antacids are given but there is rarely much improvement in the ulcers. They do seem to prevent ulcers getting worse, however so may be useful at times of stress. Sucrulfate is often used in combination with other drugs especially to treat glandular disease.
