Liver Disease in Horses
The liver has many important functions including protein metabolism, toxin neutralisation, producing clotting factors and proteins for the blood and vitamin and mineral metabolism to name but a few. The liver also produces bile which flows through channels in the liver and then through a duct into the small intestine to neutralise the acid produced in the stomach. The liver is capable of regeneration and repair if it is damaged but extensive or repetitive damage can exhaust this ability to repair, eventually resulting in liver failure. Clinical signs of liver failure are not seen until more than 70% of the liver’s function is compromised and hence many cases of liver disease are subclinical or only exhibit very mild signs.
Clinical Signs (Rarely all these signs together!)
- Weight loss
- Anorexia (reluctance to eat)
- Depression / grumpiness
- Colic (this may be recurrent)
- Jaundice
- Hepatic encephalopathy :- Head pressing, walking aimlessly, frequent yawning, circling, blindness
- Photosensitisation (sunburn)
- Itchy and/or scaly skin
- Drinking and urinating increased volumes of fluid
- Swollen sheath / pad of fluid along belly (Ventral oedema)
- Poor performance

Ragwort.
Causes
- Ragwort poisoning
- Other toxic plants e.g. St John’s Wart
- Mycotoxins/feed toxins
- Iron toxicity
- Bacterial infection (including abscesses)
- Mycotoxins / Other toxins
- Parasites (worms and flukes)
- Metabolic (secondary to Equine Metabolic Syndrome and Cushing’s)(PPID)
- Active hepatitis (inflammation with no obvious cause)
- Tumours / Bile stones (choleliths) obstructing the bile ducts
- Hyperlipaemia
Diagnosis
Blood tests; there are a number of enzymes produced by the liver which are found in increased volumes in the blood stream if the liver is damaged, these are called AST and GLDH. Another enzyme called GGT is elevated when the bile flow through a damaged liver is impaired.
Any of the commonly measured indices that are run on routine blood tests (haematology and biochemistry) can be altered in horses suffering from liver disease because the liver has so many varied functions making it particularly important to run a full blood profile.
If initial results indicate liver disease we will use a specialist laboratory to measure bile acids which provide a good indication of liver function.
Sometimes horses are diagnosed with liver disease when blood tests are run for other conditions.
When assessing a horse with signs of liver disease our aim is to determine three fundamental things:
- if there is genuine liver damage,
- what is the likely cause of liver damage and;
- what is the prognosis (likelihood of recovery) for the individual concerned.
The best technique we have to answer these questions is to take a liver biopsy. Biopsies are particularly useful for evaluating diffuse disease and aiding us in assessing prognosis. Biopsies may miss focal disease like an abscess but the chances of sampling the right area can be increased by using ultrasound to select the area to be sampled.
A liver biopsy is taken using local anaesthetic at the biopsy site on a sedated (standing) horse. This is a very safe procedure, the small risks involved include internal bleeding, introduction of infection and damage to other organs; using ultrasound guidance we can minimise these risks.
Forage analysis can be useful to identify mycotoxins.
Treatment
Treatment is targeted in 4 ways;
- Treating the cause of liver disease, if known
- Treating the symptoms
- Supporting recovery of the liver
- Supporting other body systems suffering the knock on effects of liver disease
Treatments targeting the direct cause of liver disease include the use of antibiotics if bacterial infection is involved and steroids if there is infiltrative disease; anti inflammatories are sometimes dispensed. Damage caused by ragwort poisoning cannot be reversed so treatment is aimed at managing the symptoms and preventing further damage. Ponies with Equine Metabolic Syndrome (EMS) or Cushing’s (PPID) often have secondary liver problems. Therefore, by supporting the liver and controlling EMS or PPID, the liver will often recover. We regularly supply and prescribe supplements to support liver function and optimise gut function.
 Thin horse.
Thin horse.
Emergency Treatment
Horses exhibiting severe symptoms such as, anorexia, colic, blindness, seizures, abnormal behaviour and head pressing (due to hepatic encephalopathy) and photosensitization require emergency and intensive treatment as these symptoms can be fatal or at the very least extremely painful. Hepatic encephalopathy is caused by abnormally high levels of ammonia in the blood stream which is toxic to the brain and affects the nervous system which can result in permanent damage to the nervous system. We may treat this by giving lactulose by mouth which absorbs excess ammonia in the gut and prevents it going into the blood stream. We can also give concentrated saline by drip into the blood stream which draws water off of the brain and can lead to a rapid improvement in clinical signs (this is rarely necessary).
Anorexia is of particular concern in horses with liver disease because if the horse has not eaten for a couple of days body fat starts to be mobilised and has to be processed by the liver before it is turned into useful calories. This extra demand on an already compromised liver can exacerbate clinical signs and increase damage to liver cells. The liver cannot deal with certain types of fat and small ponies and donkeys in particular are sometimes seen to develop a serious complication called hyperlipaemia that can be fatal. If we cannot persuade a horse to eat then we have to give nutrients, particularly glucose, directly into the blood stream or via stomach tube.
Weight loss
Weight loss is attributed to poor utilisation of nutrients as the liver is failing to process them properly and a general feeling of malaise. Supplementing vitamins by injection and in feed can make a rapid difference to a horse’s demeanour. See feeding for more details.
Photosensitisation
Horses that have become photosensitive get sunburnt skin beneath the white patches of fur in their coat. This usually develops first on their noses and legs but can occur anywhere on the body where there is white hair. In mild cases the skin will be red and sore to touch initially and then become scabby and produce an oily yellow discharge, severely burnt skin becomes like dried leather and forms wrinkles in the coat, such areas become extremely painful to touch.
Photosensitised horses can get sun burnt in the middle of winter and on days when there is complete cloud cover!
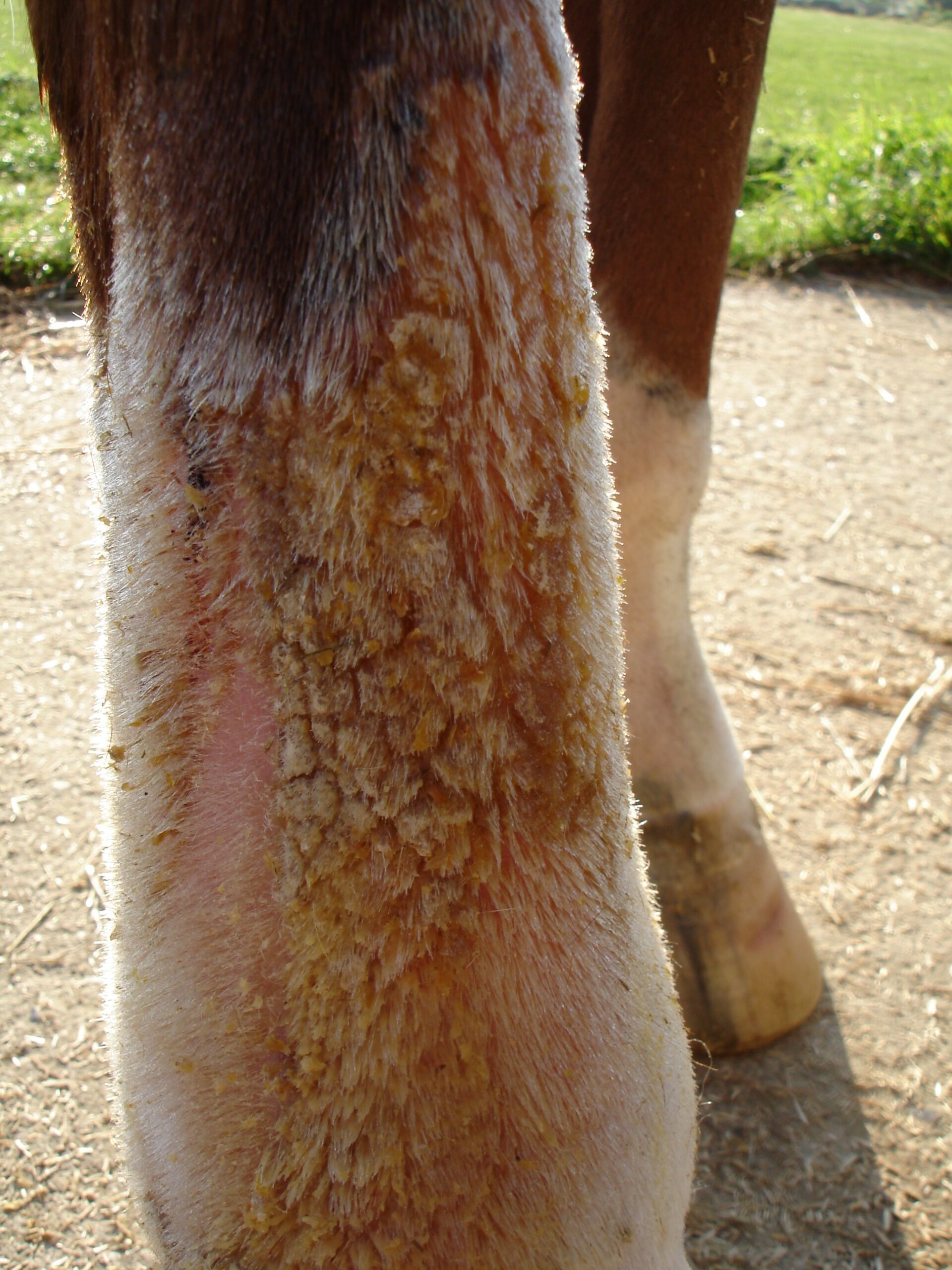 Sore skin – photosensitised.
Sore skin – photosensitised.
If a horse develops sun burn because of photosensitisation due to liver disease it must be kept in a stable with the windows blacked out and door completely shut during all daylight hours and pain-relieving drugs will need to be administered.
Photosensitisation occurs when the liver is unable to process chlorophyll (green pigment in plants). An intermediate metabolite of this process reacts with the UV light in sunlight to produce toxic radicals that cause severe tissue damage.
Feeding the horse with liver disease
Feeding a horse with liver disease is a tricky balancing act between giving enough protein and energy to prevent weight loss whilst minimising the work the liver has to do to metabolise that protein. Overall grass is best (Turnout at night for photosensitised horses).
The basic principles to follow are;
- Avoid feeds containing high levels of crude protein e.g. alfalfa, soyabean meal, clover.
- Avoid haylage
- Avoid grains (other than cracked / flaked oats and maize).
- Some complete pure high fibre diet pellets are ok.
- Sugar beet and wheat bran are OK
- Feed little and often (5-6 times a day if requiring weight gain)
- Provide ad lib high quality fibre e.g. grass or hay (avoid alfa afla hay)
But your vet may prescribe a more specific direct tailored to your horse.
In addition to supplements we prescribe, consider having hay analysed.
Vitamin and mineral supplementation including zinc and vitamins B, K and folic acid is important because these vitamins are all made in the liver and their production is compromised in sick livers. Storage of vitamins A, D and E may be reduced in liver disease, but excessive supplement is to be avoided.
Excessive copper and iron should be avoided as iron is toxic to livers. Zinc supplement may be necessary. The perfect vitamin supplement does not exist but we use weekly pastes.
Feeding oil may be beneficial if weight gain is required.
Suggested diet for a horse with a compromised liver would be;
Ad-lib hay and grass if thin (restricted if over weight/at high risk of getting laminitis). Hay is better than haylage but high fibre haylage is ok.
If grass is short and intake of hay is too low then Readigrass is a good addition.
For a laminitic risk pony, unmolassed sugar beet can be used (adlib sugar beet is avoided due to high Ca level). Total feed intake around 1 – 1.5% bodyweight, but mostly fibre (Hay soaked for 1 hour)
It is more important to keep a horse eating (trickle feeding preferable) than adjust diet and depress appetite.
For individual advice, ask your vet.
Last reviewed July 2022
